We need to talk about continence poverty.
12 November 2025
Incontinence is not a subject most people feel comfortable discussing, but it is a fact of life for many older people. Perhaps reflecting the associated stigma, it has not been widely researched, especially in low and middle-income countries (Batmani et al, 2021). Yet it is far from uncommon. It has been reported that 16 per cent of people aged 60 or more living in southern Brazil experience some form of urinary incontinence (Dziekaniak, Meucci & Cesar, 2019). Incontinence can add to pressures on healthcare systems by increasing the risk of conditions like genitourinary infections, which lead to over 200,000 hospitalisations a year in Brazil (Dias & Barros, 2019).
Some types of incontinence can be mitigated in different ways, such as regular pelvic exercises (HelpAge International, 2025). But for many older people, the only realistic option to manage the condition is with products such as adult pads. The evidence is there to see in local pharmacies, which stock large amounts of adult pads. This is a photo we took earlier this year in a poor Brazilian urban neighbourhood.
Incontinence pads are not cheap. In high-income countries, the term “continence poverty” was coined a few years ago and has quickly gained profile as a policy concern (NHS England, 2018). In Brazil, some local governments offer free pads to poor families with an identified need, and earlier this year, the federal MoH adopted this as a national policy (Brasil, 2025). But whether people in need can access these pads is another question -there are several steps and hurdles to navigate.
Eligibility requires an examination by a physician and a letter certifying the degree and form of incontinence. For many older people, getting to a health centre is no easy matter, especially if they have impaired mobility and live in areas like the one in this image.
Community health workers usually make home visits, and sometimes nurses, who are not permitted to assess applicant eligibility for free pads. Very limited numbers of physicians in health centres mean older people may wait months for a home visit, if it ever happens at all. According to one local health worker we interviewed:
People tell us, “I need a visit from the doctor”, but there is so much demand. You need to have a vehicle to visit, and you have to order one in advance. We don’t have our own car in this health centre, and so you have to request the district office.
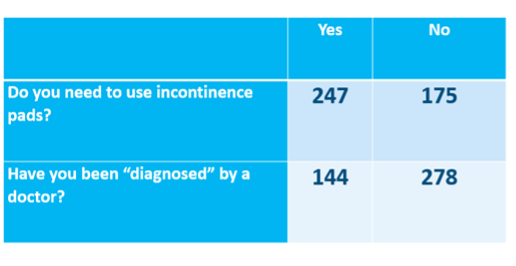
As part of our RGHI project, we have been working with the city government of Belo Horizonte in Brazil to collect data about how older people living in slum areas are affected by incontinence. Here are some preliminary findings:
As the table shows, only 144 of 247 older people who needed pads had their condition assessed by a doctor and had, presumably, been given the necessary letter.
The older person should then take the letter and proof of their identity to a local community pharmacy, where they will be given the pads. For older people with impaired mobility, this presents the same logistical challenges as getting to a local health centre, and pharmacies do not make home deliveries. Theoretically, another person can go on the applicant’s behalf, but only if they are formally recognised as this person’s representative, which requires a separate legal process. In some cases, pharmacies limit each collection to a 10-day supply of pads, requiring three visits a month. And after six months, it is necessary to renew the physician’s assessment and repeat the application process.
Unsurprisingly, many of the older people in our study have not been able to obtain free pads and are left with a choice between buying their own or doing without. Here is a typical experience related by a local care worker:
I work with an old woman who lives on her own and has urinary incontinence. The social workers have been trying to get free pads for her, but haven’t succeeded so far, and so she has to buy her own. But she’s really reluctant to use them and just lets the urine go where it will. I spent a year trying to persuade her to use pads, but she says they are just too expensive for her.
Other informants have told us about older people minimising the amount they drink to reduce their need for pads. This then causes dehydration, which leads to serious health problems such as kidney disease.
All of us -researchers, policymakers and the general public- need to be more aware of these issues and more open to discussing them. In the case of Brazil, this might include asking why the need for continence pads can be confirmed only by physicians, rather than by other health professionals. Also, there may be opportunities to distribute pads directly to the homes of those in need, through community health workers. Brazil’s Ministry of Health is to be congratulated for its new policy, and hopefully, there will be opportunities to strengthen it in the near future.
Peter Lloyd-Sherlock, Renan Amaral, Jesilaine Barbosa, Wanderson Bomfim, Karla Giacomin, Larissa Pedreira, Poliana Fialho do Carvalho and Roberta Goes.
References:
Batmani, S et al (2021). Prevalence and factors related to urinary incontinence in older adult women worldwide: a comprehensive systematic review and meta-analysis of observational studies. BMC Geriatr 21, 212.
Brasil M (2025) Fraldas geriátricas passam a ser gratuitas na Farmácia Popular. https://www.em.com.br/nacional/2025/02/7060377-fraldas-geriatricas-passam-a-ser-gratuitas-na-farmacia-popular.html
Dias R & Barros J (2019) Burden of hospitalisation among older people in the Brazilian public health system: a big data analysis from 2009 to 2015. J Epidemiol Community Health 73(6):537-543.
Dziekaniak A, et al (2019) Urinary incontinence among older adults living in the rural area of a municipality in southern Brazil. Geriatr Gerontol Aging. 13:4-10.
HelpAge International, 2025. Toolkit for home-based incontinence care. Supporting older women and men, and their caregivers, in low resource settings. https://knowledge-action-portal.com/en/content/toolkit-homebased-incontinence-care
NHS England, 2018. Excellence in Continence Care. Practical guidance for commissioners, and leaders in health and social care. https://www.england.nhs.uk/wp-content/uploads/2018/07/excellence-in-continence-care.pdf
Peter LLoyd-Sherlock, RGHI Innovation Grant Award Holder